Ocular hypertension, Open-angle glaucoma
Adult: As 1% solution: Instil one drop in the affected eye(s) bid.
|
Indications and Dosage
Ophthalmic
Ocular hypertension, Open-angle glaucoma Adult: As 1% solution: Instil one drop in the affected eye(s) bid.
|
|
Administration
Should be taken with food.
|
|
Contraindications
Sinus bradycardia, 2nd- or 3rd-degree AV block, cardiogenic shock, overt cardiac failure; bronchial asthma or history of bronchial asthma, severe COPD.
|
|
Special Precautions
Patient with history of atrophy or severe anaphylaxis to different allergens, diabetes mellitus, compensated heart failure, myasthenia gravis, peripheral vascular disease, Raynaud's disease. May mask symptoms of hyperthyroidism and hypoglycaemia. Avoid abrupt withdrawal.
|
|
Adverse Reactions
Significant: Anaphylactic reactions, choroidal detachment.
Cardiac disorders: Bradycardia, arrhythmia, palpitations, syncope. Eye disorders: Transient eye irritation (e.g. burning, tearing, conjunctival hyperaemia and oedema), visual disturbance, ptosis, diplopia, photophobia. Gastrointestinal disorders: Dysgeusia, nausea. General disorders and administration site conditions: Asthenia. Investigations: Decreased blood pressure. Nervous system disorders: Headache, dizziness, insomnia. Psychiatric disorders: Depression. Respiratory, thoracic and mediastinal disorders: Bronchospasm, dyspnoea, sinusitis. Skin and subcutaneous tissue disorders: Rash. Potentially Fatal: Severe respiratory reactions (e.g. bronchospasm); cardiac failure. |
|
Ophth: C
|
|
Patient Counseling Information
Remove contact lenses prior to administration and wait for 15 minutes before reinserting.
|
|
Monitoring Parameters
Monitor for systemic effect of β-blockade with ophthalmic administration. Monitor IOP, blood pressure, heart rate.
|
|
Overdosage
Symptoms: Bradycardia, bronchospasm, congestive heart failure, and hypotension. Management: Symptomatic and supportive treatment. Flush eyes with water or normal saline solution in case of ocular overdose.
|
|
Drug Interactions
Additive hypotensive effect and/or marked bradycardia with catecholamine-depleting drugs (e.g. reserpine).
|
|
Action
Description:
Mechanism of Action: Carteolol is a long-acting, non-cardioselective beta-blocker which blocks both β1 and β2 adrenergic receptors. It reduces aqueous humour production or possibly increases aqueous humour outflow resulting in reduction of intraocular pressure (IOP). Pharmacokinetics: Absorption: Absorbed systemically after ophthalmic administration. Distribution: Plasma protein binding: Approx 20-30%. Metabolism: Metabolised in the liver by CYP2D6 to its active metabolite 8-hydroxycarteolol and glucuronic acid conjugates of carteolol and 8-hydroxycarteolol. Excretion: Via urine: Approx 50-70% (as unchanged drug). Elimination half-life: Approx 5 hours. |
|
Chemical Structure
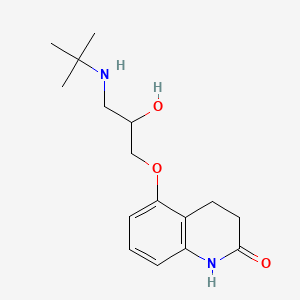 Source: National Center for Biotechnology Information. PubChem Compound Summary for CID 2583, Carteolol. https://pubchem.ncbi.nlm.nih.gov/compound/Carteolol. Accessed Mar. 22, 2024. |
|
Storage
Store between 15-25°C. Protect from light.
|
|
MIMS Class
|
|
ATC Classification
C07AA15 - carteolol ; Belongs to the class of non-selective beta-blocking agents. Used in the treatment of cardiovascular diseases.
|
|
References
Anon. Carteolol (Ophthalmic). Lexicomp Online. Hudson, Ohio. Wolters Kluwer Clinical Drug Information, Inc. https://online.lexi.com. Accessed 01/03/2024. Buckingham R (ed). Carteolol Hydrochloride. Martindale: The Complete Drug Reference [online]. London. Pharmaceutical Press. https://www.medicinescomplete.com. Accessed 01/03/2024. Carteolol Hydrochloride Ophthalmic Solution USP, 1% (Sandoz Inc). DailyMed. Source: U.S. National Library of Medicine. https://dailymed.nlm.nih.gov/dailymed. Accessed 01/03/2024. Carteolol. Gold Standard Drug Database in ClinicalKey [online]. Elsevier Inc. https://www.clinicalkey.com. Accessed 01/03/2024.
|