Chronic obstructive pulmonary disease
Adult: Maintenance: As inhalation cap: 1 cap (150 mcg) once daily via inhaler device, at the same time each day. Severe: 300 mcg once daily. Max: 300 mcg daily.
|
Indications and Dosage
Inhalation/Respiratory
Chronic obstructive pulmonary disease Adult: Maintenance: As inhalation cap: 1 cap (150 mcg) once daily via inhaler device, at the same time each day. Severe: 300 mcg once daily. Max: 300 mcg daily.
|
|
Special Patient Group
Pharmacogenomics:
Indacaterol is metabolised by uridine diphosphate glucuronosyltransferase 1 family, polypeptide A1 (UGT1A1) enzyme via glucuronidation into phenolic O-glucuronide metabolite. According to FDA-approved drug label, patients with UGT1A1 (TA)7/(TA)7 (*28/*28) low expression genotype have 1.2-fold higher steady-state AUC and Cmax than in patients with (TA)6/(TA)6 (*1/*1) genotype. This suggests that UGT1A1 genotype has no significant effect in the exposure of indacaterol. |
|
Contraindications
As monotherapy in the treatment of asthma. Concomitant use with other long-acting ß2-adrenergic agonists.
|
|
Special Precautions
Patient with CV disorders (e.g. coronary artery disease, acute MI, cardiac arrhythmias, hypertension, known or suspected QT interval prolongation); convulsive disorders, hyperthyroidism, diabetes mellitus, hypokalaemia. Pregnancy and lactation. Not indicated for the relief of acute bronchospasm.
|
|
Adverse Reactions
Significant: Hypersensitivity reactions (e.g. swelling of tongue, lips and face, rash, urticaria, difficulty in breathing or swallowing), hypokalaemia, hyperglycaemia, new-onset or exacerbation of diabetes mellitus, increased pulse rate or blood pressure, ECG changes (e.g. flattening of T wave, QT interval prolongation, ST-segment depression).
Cardiac disorders: Chest pain, palpitations, tachycardia. Metabolism and nutrition disorders: Peripheral oedema. Musculoskeletal and connective tissue disorders: Muscle spasm, musculoskeletal pain. Nervous system disorders: Headache, dizziness. Respiratory, thoracic and mediastinal disorders: Upper respiratory tract infection, nasopharyngitis, sinusitis, cough, oropharyngeal pain, rhinorrhoea. Potentially Fatal: Paradoxical bronchospasm. |
|
Inhalation/Respiratory: C
|
|
Monitoring Parameters
Monitor forced expiratory volume in the 1st second (FEV1), forced vital capacity (FVC), other pulmonary function tests; serum K, blood glucose, blood pressure, heart rate. Monitor deterioration of COPD and re-evaluate therapy as needed.
|
|
Overdosage
Symptoms: Increased pulse rate, systolic blood pressure, QTc interval; other exaggerated adverse effects (e.g. tachycardia, palpitations, headache, ventricular arrhythmias, hypokalaemia, hyperglycaemia). Management: Supportive and symptomatic treatment. Administer cardioselective β-blockers under physician supervision. Monitor cardiac function.
|
|
Drug Interactions
Sympathetic effects may be potentiated with sympathomimetic agents. Enhanced hypokalaemic effect of methylxanthine derivatives, steroids or non-potassium-sparing diuretics (loop or thiazide diuretics). Increased risk of prolonged QTc interval with MAOIs, TCAs, or other agents known to prolong QTc interval. Antagonistic effect with ß-adrenergic blockers. Increased serum concentration with inhibitors of CYP3A4 and P-glycoprotein (e.g. ketoconazole, erythromycin, verapamil, ritonavir).
|
|
Action
Description:
Mechanism of Action: Indacaterol is a long-acting β2-adrenergic agonist. It acts by stimulating intracellular adenyl cyclase thus increasing the level of cyclic 5’-adenosine monophosphate (AMP) resulting in the relaxation of bronchial smooth muscle. Indacaterol is a long-acting ß2-adrenergic agonist. It acts by stimulating intracellular adenyl cyclase thus increasing the level of cyclic 5’-adenosine monophosphate (AMP) resulting in the relaxation of bronchial smooth muscle. Onset: 5 minutes. Duration: 24 hours. Pharmacokinetics: Absorption: Bioavailability: 43-45%. Time to peak plasma concentration: Approx 15 minutes. Distribution: Volume of distribution: 2,557 L (IV). Plasma protein binding: Approx 95%. Metabolism: Metabolised in the liver by CYP3A4, CYP2D6 and CYP1A1 to hydroxylated indacaterol and by UGT1A1 to phenolic O-glucuronides. Excretion: Via faeces (>90%; 54% as unchanged drug, 23% as hydroxylated metabolites); urine (<2% as unchanged drug). Elimination half-life: 40-56 hours. |
|
Chemical Structure
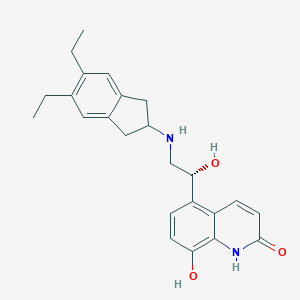 Source: National Center for Biotechnology Information. PubChem Database. Indacaterol, CID=6918554, https://pubchem.ncbi.nlm.nih.gov/compound/Indacaterol (accessed on Jan. 21, 2020) |
|
Storage
Store below 30°C. Protect from light and moisture.
|
|
MIMS Class
|
|
ATC Classification
R03AC18 - indacaterol ; Belongs to the class of adrenergic inhalants, selective beta-2-adrenoreceptor agonists. Used in the treatment of obstructive airway diseases.
|
|
References
Annotation of FDA Label for Indacaterol and UGT1A1. Pharmacogenomics Knowledgebase (PharmGKB). https://www.pharmgkb.org/. Accessed 14/11/2019. Annotation of PMDA Label for Indacaterol and UGT1A1. Pharmacogenomics Knowledgebase (PharmGKB). https://www.pharmgkb.org/. Accessed 15/11/2019. Anon. Indacaterol. Lexicomp Online. Hudson, Ohio. Wolters Kluwer Clinical Drug Information, Inc. https://online.lexi.com. Accessed 14/11/2019. Anon. UGT1A1 - Indacaterol (Pharmacogenomics). Lexicomp Online. Hudson, Ohio. Wolters Kluwer Clinical Drug Information, Inc. https://online.lexi.com. Accessed 15/11/2019. Arcapta Neohaler (Sunovion Pharmaceuticals Inc.). DailyMed. Source: U.S. National Library of Medicine. https://dailymed.nlm.nih.gov/dailymed/. Accessed 14/11/2019. Arcapta Neohaler Capsule (Novartis Pharmaceuticals Corporation). DailyMed. Source: U.S. National Library of Medicine. https://dailymed.nlm.nih.gov/dailymed/. Accessed 10/09/2014. Buckingham R (ed). Indacaterol. Martindale: The Complete Drug Reference [online]. London. Pharmaceutical Press. https://www.medicinescomplete.com. Accessed 14/11/2019. McEvoy GK, Snow EK, Miller J et al (eds). Indacaterol Maleate. AHFS Drug Information (AHFS DI) [online]. American Society of Health-System Pharmacists (ASHP). https://www.medicinescomplete.com. Accessed 10/09/2014. Novartis New Zealand Limited. Onbrez Breezhaler 150 mcg Inhalation Powder Hard Capsules data sheet 15 September 2017. Medsafe. http://www.medsafe.govt.nz/. Accessed 14/11/2019.
|